Supplements for ADHD: what looks promising, what may help, and what is probably overhyped
A whole-body look at saffron, pine bark extract, melatonin, omega-3s, gut-targeted supplements, vitamin D, magnesium and L-theanine, for starters…
When people ask me whether supplements help with ADHD, I rarely begin by telling them whether a supplement “works”. I start somewhere else. In fact, I may ask what, exactly, they are trying to support. Is it attention, sleep, or emotional regulation? Maybe it’s appetite, nutritional status or digestive symptoms? And then there’s the inescapable accumulated wear and tear of living in a nervous system that has had to work very hard for a very long time?
It would be much easier to say yes or no and then cite a series of studies to show off how much I have read. But, as a good ADHDer, I prefer longer answers. Sorry, not sorry! In fact, my favourite answers are the ones that make us rethink the question itself, because when the question improves, the conversation usually improves too.
This matters, a lot, because ADHD is not one single “thing”. It is not just hyperactivity or inattention, so it rarely makes sense to approach it from one angle alone. In my experience, it is very easy to end up with two equally unhelpful stories. In one, supplements are dismissed completely. In the other, their effectiveness is inflated into a kind of nutritional redemption, as if capsule X could replace medication, movement, sleep, therapy, creativity, self-understanding, and the practical scaffolding so many of us genuinely need. I do not agree with either version.
So, yes, I think some supplements deserve consideration, and some are promising. But I do not think supplements replace medication or any other therapeutic approach for ADHD. The evidence base for stimulants in adults remains much stronger than the evidence base for supplements when we are talking about core ADHD symptoms. Serious and internationally respected clinical guidelines such as NICE, the National Institute for Health and Care Excellence in the UK, still recommend methylphenidate or lisdexamfetamine as first-line pharmacological treatment for adults when medication is indicated. At the same time, broader care still matters, and NICE is clear that ADHD management is not only about pharmacological treatment. ¹
What does the evidence say about saffron, omega-3s, melatonin, probiotics, magnesium and other nutritional supplements?
When I read studies on supplements, I do not simply ask whether the result is positive. I look at whether the study was done in children or adults, whether it was a pilot or a larger trial, ideally randomised and blinded, or whether it was an open-label, non-randomised study. I also think it matters whether the supplement was used as a standalone treatment or as an add-on, and what hypothesis the study was built around.
ADHD is not only about dopamine, focus and hyperactivity. From my perspective, a well-designed study should investigate the supplement’s effects on sleep, mood, behaviour and oxidative stress, as well as core ADHD symptoms. Then there’s the demographics. If a study only includes boys and not girls, or if a study only includes adult men, it becomes much harder to generalise the findings to women. These details matter far more than people often realise, because they tell us how far a finding can reasonably travel beyond the original sample.
Omega-3
Omega-3s still deserve to be part of the conversation, but the story needs to be taken with a pinch of salt, as we say in English. Fish oils, or algal oils for people who prefer not to consume animal products, are among the most researched supplements in ADHD, and that is one of the reasons they keep appearing in the conversation. The problem is that “one of the most researched” is often confused with “clearly effective”.
The Cochrane Collaboration, an independent international non-profit network that produces high-quality systematic reviews on health interventions, published an update in 2023. Its conclusion was that, overall, there was little evidence that supplementation with polyunsaturated fatty acids improved ADHD symptoms in children and adolescents. ²
A meta-analysis published that same year also found no significant overall effect on core ADHD symptoms, although longer trials, lasting at least four months, seemed somewhat more promising. In that case, the possible advantage still referred to core ADHD symptoms themselves, not to broader benefits, such as cardiovascular benefits. The study also does not allow us to say clearly which specific dimension, inattention, hyperactivity or impulsivity, benefited most. ³
That said, not all the literature points in the same direction. An earlier meta-analysis by Chang et al. found that omega-3 supplementation could modestly improve clinical ADHD symptoms and some attention-related cognitive measures in children and adolescents. It also observed that young people with ADHD tended to have lower levels of DHA, EPA and total omega-3s than controls. ⁴ This does not invalidate the more cautious reviews, but it does force us to avoid binary messages. For me, the most honest reading is that there may be a real, though small, signal, especially in children and adolescents and perhaps in longer interventions, without this justifying the presentation of omega-3s as a powerful intervention or the direct extrapolation of these findings to adults.
Omega-3s: My veredict
For me, omega-3s still make sense as a foundational support, with anti-inflammatory and neurobiological plausibility, but not as a strong or clearly transformative intervention by themselves.
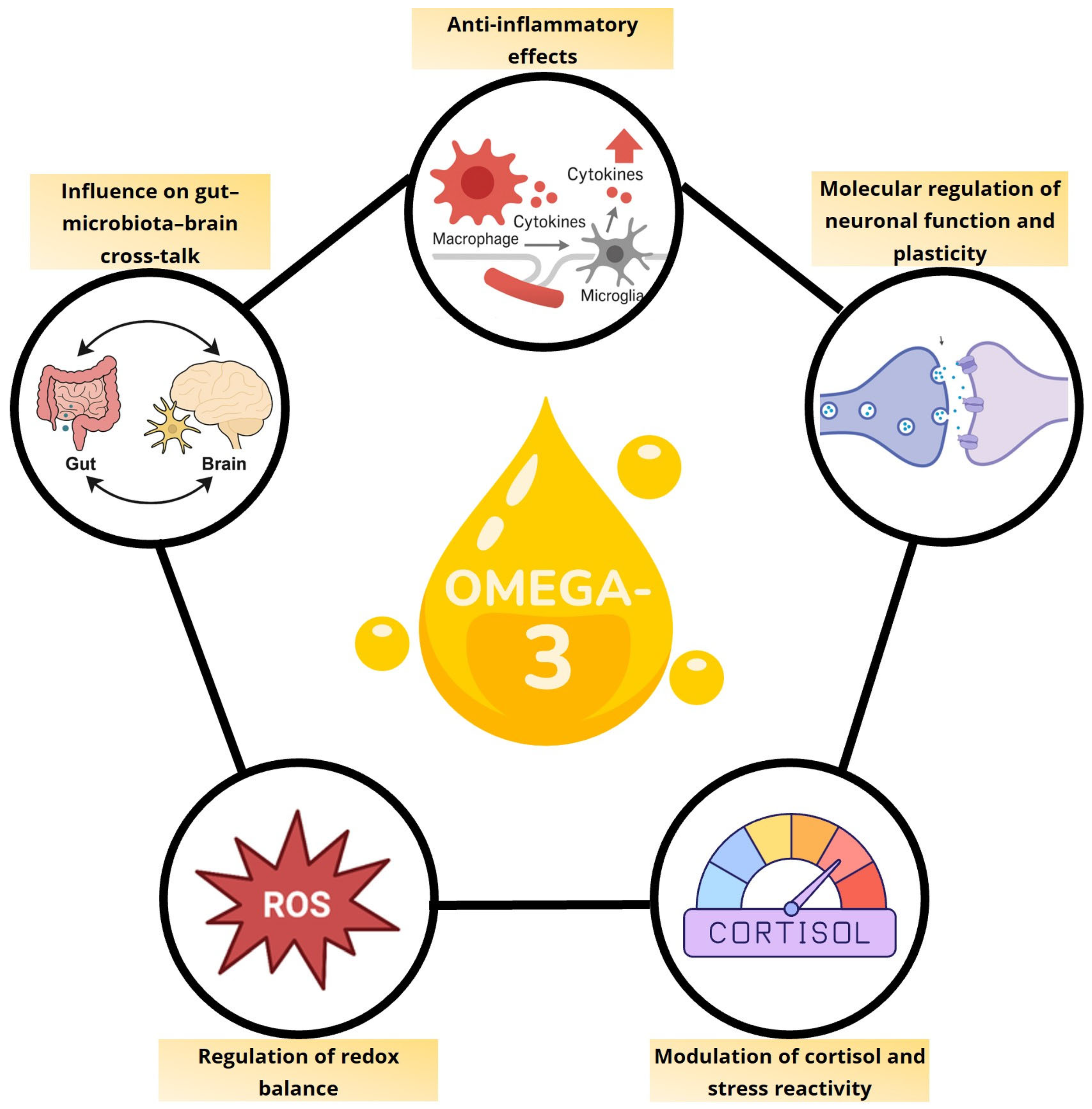
Although omega-3s do not appear to be the “miracle” for ADHD that is sometimes promised, they remain relevant nutrients because of their involvement in inflammation, oxidative stress, stress response, neuronal plasticity and the gut-microbiota-brain axis. Their value may not lie in a spectacular effect on symptoms on their own, but in their capacity to support a more regulated biological terrain, something I will explore in more detail in future articles.
Figure adapted from: De Cillis et al., Nutrients, 17(21), 3426, under a Creative Commons CC BY 4.0 licence.
Saffron
Saffron is one of the most interesting supplements in this area, and I think it deserves serious attention. But I also think it is a good example of why methodology matters.
The 2019 Baziar study is often cited because it directly compared saffron with methylphenidate in children and adolescents. ⁵ That is clinically bold and genuinely interesting, but we also need to see it for what it is: a six-week, double-blind pilot study in a small paediatric sample. A positive result in children does not automatically tell me that the same extract will behave in the same way in adults, with a different hormonal environment, other coexisting conditions, different sleep patterns, different medication exposure, and, above all, different life demands. What it tells me is that saffron deserves to be taken seriously, not that the question in adults has already been resolved.
A later study, Blasco-Fontecilla 2022, is striking for another reason. It used both objective tests and paper-and-pencil measures, which I like to see, but it was not randomised. The methylphenidate group included 27 participants and the saffron group included 36, all aged between 7 and 17. ⁶
The main finding was that saffron appeared, broadly speaking, comparable to methylphenidate, with saffron seeming stronger for hyperactivity and methylphenidate stronger for inattention. Another interesting signal, but the non-randomised design means I would be careful not to treat it as more robust than it is. Even so, the research team is excellent, and from where I stand, the study adds texture to the literature. A little like saffron adds colour to a good paella, even if it is not the main ingredient.
Saffron has something especially evocative in the Spanish context, and even more so in La Mancha, where it forms part of the landscape, the cuisine and the cultural memory. Although it probably did not arrive in the Iberian Peninsula exclusively through the Arab world, it does seem clear that its expansion and deep rooting in Spain were closely linked to the Andalusian period. I like to think of this as a symbol of something wider too: how many of the things we now feel as deeply ours were actually born from exchange between cultures. Perhaps that is why saffron, as well as being beautiful and valuable, feels like a bridge between history, land and knowledge.
The adult saffron trial that feels most clinically relevant to me, precisely because it stops us leaning too heavily on child data, is the 2022 study by Pazoki and colleagues. Again, the most important detail is that this was an add-on trial. Fifty-six adults were randomly assigned to receive Ritalin with saffron or Ritalin with placebo for six weeks, and 44 completed the study. The saffron group showed a greater reduction in ASRS scores, with significant time-by-treatment effects also seen in the Conners’ Adult ADHD Rating Scales, CAARS. This does not confirm that saffron can replace stimulant treatment in adults, but it does give us an indication that methylphenidate combined with saffron may offer an interesting angle of support. It is a narrow conclusion, but an honest one. ⁷
El azafrán es uno de los suplementos más interesantes en este ámbito, y creo que merece atención seria. Pero también creo que es un buen ejemplo de por qué la metodología importa. El estudio de Baziar de 2019 se cita a menudo porque comparó directamente azafrán con metilfenidato en niños y adolescentes. ⁵ Eso es “clínicamente atrevido” y realmente interesante, pero también hay que verlo por lo que es: un piloto doble ciego de seis semanas en una muestra pequeña y pediátrica. Un resultado positivo en niños no me dice automáticamente que el mismo extracto vaya a comportarse igual en adultos, con un entorno hormonal distinto, otras condiciones coexistentes, otros patrones de sueño, otra exposición a medicación y, sobre todo, otras exigencias vitales. Lo que me dice es que el azafrán merece ser tomado en serio, no que la cuestión en adultos esté ya resuelta.
Un estudio posterior (Blasco-Fontecilla, 2022) es llamativo por otra razón. Utilizó tanto pruebas objetivas como medidas en papel y lápiz, algo que me gusta ver, pero no fue aleatorizado, con metilfenidato en 27 participantes y azafrán en 36, todos entre 7 y 17 años. ⁶ El hallazgo principal fue que el azafrán parecía, en términos generales, comparable al metilfenidato, con el azafrán pareciendo más fuerte para la hiperactividad y el metilfenidato más fuerte para la inatención. Otra señal interesante, pero el diseño no aleatorizado significa que yo tendría cuidado de no tratarlo como algo más robusto de lo que es. Aun así, el equipo de investigación es excelente, y el estudio, desde donde yo lo veo, añade textura a la literatura. Un poco como el azafrán añade color a una buena paella, aunque no sea el ingrediente principal.
Saffron has something especially evocative in the Spanish context, and even more so in La Mancha, where it forms part of the landscape, the cuisine and the cultural memory. Although it probably did not arrive in the Iberian Peninsula exclusively through the Arab world, it does seem clear that its expansion and deep rooting in Spain were closely linked to the Andalusian period. I like to think of this as a symbol of something wider too: how many of the things we now feel as deeply ours were actually born from exchange between cultures. Perhaps that is why saffron, as well as being beautiful and valuable, feels like a bridge between history, land and knowledge.
The adult saffron trial that feels most clinically relevant to me, precisely because it stops us leaning too heavily on child data, is the 2022 study by Pazoki and colleagues. Again, the most important detail is that this was an add-on trial. Fifty-six adults were randomly assigned to receive Ritalin with saffron or Ritalin with placebo for six weeks, and 44 completed the study. The saffron group showed a greater reduction in ASRS scores, with significant time-by-treatment effects also seen in the Conners’ Adult ADHD Rating Scales, CAARS. This does not confirm that saffron can replace stimulant treatment in adults, but it does give us an indication that methylphenidate combined with saffron may offer an interesting angle of support. It is a narrow conclusion, but an honest one. ⁷
What is the ASRS?
The ASRS-v1.1, Adult ADHD Self-Report Scale, is an 18-item self-report screening questionnaire developed by the World Health Organization. It is designed to identify ADHD symptoms in adults aged 18 and over. It helps detect signs of inattention and hyperactivity/impulsivity in order to determine whether a full clinical assessment may be appropriate. On my adult ADHD screening page, you will find a free online version that you can complete to help you understand your neurotype.
The broader reviews on saffron are encouraging, but they also show how early this field still is. A 2024 systematic review of saffron in ADHD included only four studies and 118 participants in total. ⁸ Another broader 2024 review on saffron in neurological and psychiatric conditions concluded that saffron was not inferior to conventional drugs in several areas, including ADHD, but that kind of statement can sound more decisive than the ADHD dataset really allows.
My own reading is that saffron is one of the most credible options, especially when mood, sleep or emotional regulation form part of the picture, although the evidence is still limited.
Saffron: My verdict
For me, saffron is one of the most interesting and credible options in this field, especially as a well-tolerated support, although not yet as a fully established treatment for adult ADHD.
What is interesting about saffron is not only whether it improves particular symptoms, but that it seems to touch several systems at once: inflammation, neuroprotection, microbiota, the gut barrier and gut-brain signalling. In a picture as complex and embodied as ADHD, that broader biological map matters too. For these reasons, saffron continues to seem like a very interesting intervention while the evidence supporting it continues to develop.
Figure reproduced from:Cerdá-Bernad et al., Nutrients, 14(24), 5368, under a Creative Commons CC BY 4.0 licence.
As a personal anecdote, after reading these studies, I started taking saffron alongside my daily methylphenidate and I have noticed that it works better for me, with fewer peaks and troughs, in a more stable way.
Pine bark extract
Pine bark extract, usually referred to as Pycnogenol, although this is a registered trademark, is another interesting case, especially because I always find myself wondering: “Who was the first person to pulverise pine bark and give it to someone as a nutritional supplement to see what happened?” I find that both funny and amazing.
The paediatric literature on pine bark extract is broader than the adult literature. One of the earliest trials, published in 2006, included 61 children who received 1 mg/kg/day for one month. ¹⁰ Later work, including a 2021 double-blind crossover study in 20 children across two four-week phases with a two-week washout, continued to suggest possible benefits for inattention, impulsivity and oxidative balance. ¹¹
There is also a 2022 randomised trial lasting ten weeks, in which teachers reported improvements in total ADHD score and in hyperactivity or impulsivity with both pine bark extract and methylphenidate compared with placebo, while methylphenidate showed a clearer advantage for inattention. ¹²
In addition, a second analysis from the same trial explored markers of oxidative stress and immunity, as well as changes in appetite and weight. I find this interesting not because it proves one single, neat mechanism, but precisely because it reminds us that these kinds of compounds touch several physiological layers at once. At the same time, the authors themselves could not firmly confirm an overall improvement in antioxidant or immune status, so I would read this more as a clue of biological complexity than as a closed mechanistic demonstration. ¹³ My professional judgement as a researcher is that all of this deserves attention.
The adult study on pine bark extract, however, is where the question of generalisation becomes especially important. In the 2002 crossover trial, 24 adults aged between 24 and 53 received Pycnogenol, methylphenidate and placebo in randomised order, each for three weeks. ¹⁴ Although symptoms improved during treatment, neither methylphenidate nor Pycnogenol outperformed placebo on the main outcomes. That does not mean pine bark extract does nothing. It means the evidence in adults is scarce and much less clear than the evidence in children. It also means we should not move from “promising in children” to “works in adults” as if that step did not require its own evidence, although this does not deny that pine bark extract may have a range of potential benefits beyond the brain and nervous system.
Pine bark extract: My verdict
For me, pine bark extract is interesting not only because of what it might contribute to some symptoms, but because it points towards a broader form of support that recognises that ADHD is not lived only in the brain, but in the whole body.
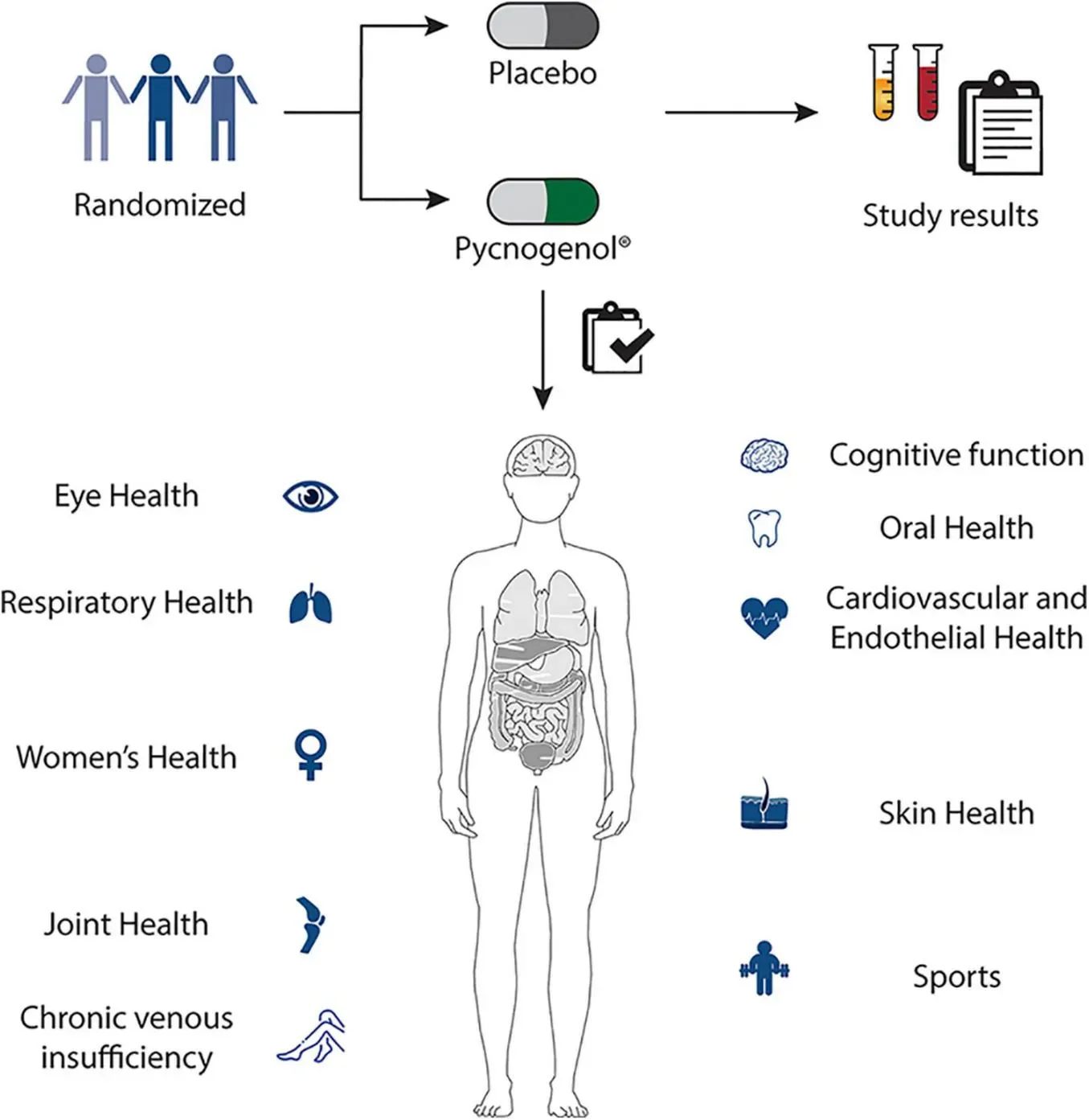
My interest in pine bark extract in ADHD is not limited to core symptoms. As with other bioactive compounds, its potential lies in the range of systems it seems to act upon, from cognitive function and vascular health to inflammatory and broader regulatory processes. In a picture as bodily as ADHD, from where I stand, that also deserves attention.
Figure adapted from: Shaw et al., Frontiers in nutrition, 11, 1389374, under a Creative Commons CC BY 4.0 licence.
Melatonin
A quick note before we begin: while melatonin is sold in many countries as a food supplement or over-the-counter sleep aid, in the UK it is a prescription-only medicine. For that reason, what follows is purely educational and is not intended as personal medical advice or a recommendation to take it.
Melatonin is best understood, in my opinion, as a support for sleep and circadian rhythm rather than as a central supplement for ADHD, and this distinction matters. In an open-label study in a small sample of children and adolescents with ADHD who were already taking psychostimulants, a small dose of melatonin, 1 mg, increased total sleep time from 463 to 485 minutes after one month, alongside a trend towards improvement in other sleep variables. ¹⁵ This is a useful study, yes, but not the type of design from which I would claim that melatonin “treats ADHD”. Rather, it suggests a sleep-supporting role in a specific context.
The chronotherapy work in adults is more interesting to me because it starts from the fact that adults with ADHD show greater susceptibility to delayed sleep phase syndrome. In other words, melatonin production starts later than it does in neurotypical people. Low doses of melatonin seem to advance the circadian rhythm, reducing self-reported ADHD symptoms by up to 14% immediately after supplementation, although the effect fades a few weeks after the treatment ends. ¹⁶
This tells me two things. First, that some of the suffering associated with ADHD is, in some cases, a rhythm problem. Second, that melatonin is most relevant when circadian phase delay is genuinely part of the picture, not as a universal intervention for everyone with ADHD.
The broader review on sleep interventions in children points in the same direction. Sleep interventions can improve sleep and, sometimes, ADHD-related variables, but the evidence is heterogeneous. ¹⁷ I find this review valuable because it takes us away from the reflex of thinking about sleep as secondary in ADHD. What it shows is that when sleep improves, not only can rest improve, but so can quality of life and, in some cases, aspects of the clinical picture itself. I also like it because, as a review, it does not sell clean or universal solutions. Instead, it shows a useful, promising and still quite heterogeneous field.
Melatonin: My verdict
For me, melatonin makes most sense when sleep and circadian rhythm are part of the problem, more as a regulatory support for the body-mind relationship than as a direct ADHD treatment. I take it myself and feel that it helps me rest better. This is what I think benefits me, more than any specific effect on my symptoms.
L-theanine
If we continue talking about circadian rhythms, sleep and rest, I would apply the same caution to L-theanine. I understand why it attracts so many people. It sits in that space of calm without sedation that many of us who live with ADHD are looking for, although the evidence in this field remains narrow.
In one of the best-known trials, supplementation with 400 mg daily helped improve some aspects of objective sleep quality in children with ADHD. Children, not adults, and sleep quality rather than the broader ADHD picture. ¹⁸
A 2024 systematic review of L-theanine in mental disorders also confirms that this amino acid, found in green tea, may help as an adjunct in situations where poor sleep, overstimulation or stress reactivity form part of the picture, but not as a main evidence-based treatment for adult ADHD. ¹⁹
L-theanine: My verdict
For me, L-theanine is more of a gentle support for creating a slightly calmer, more regulated and perhaps more habitable inner terrain than a primary intervention for adult ADHD.
Personally, I am very much “team L-theanine”, and I have taken it every afternoon or evening for years.
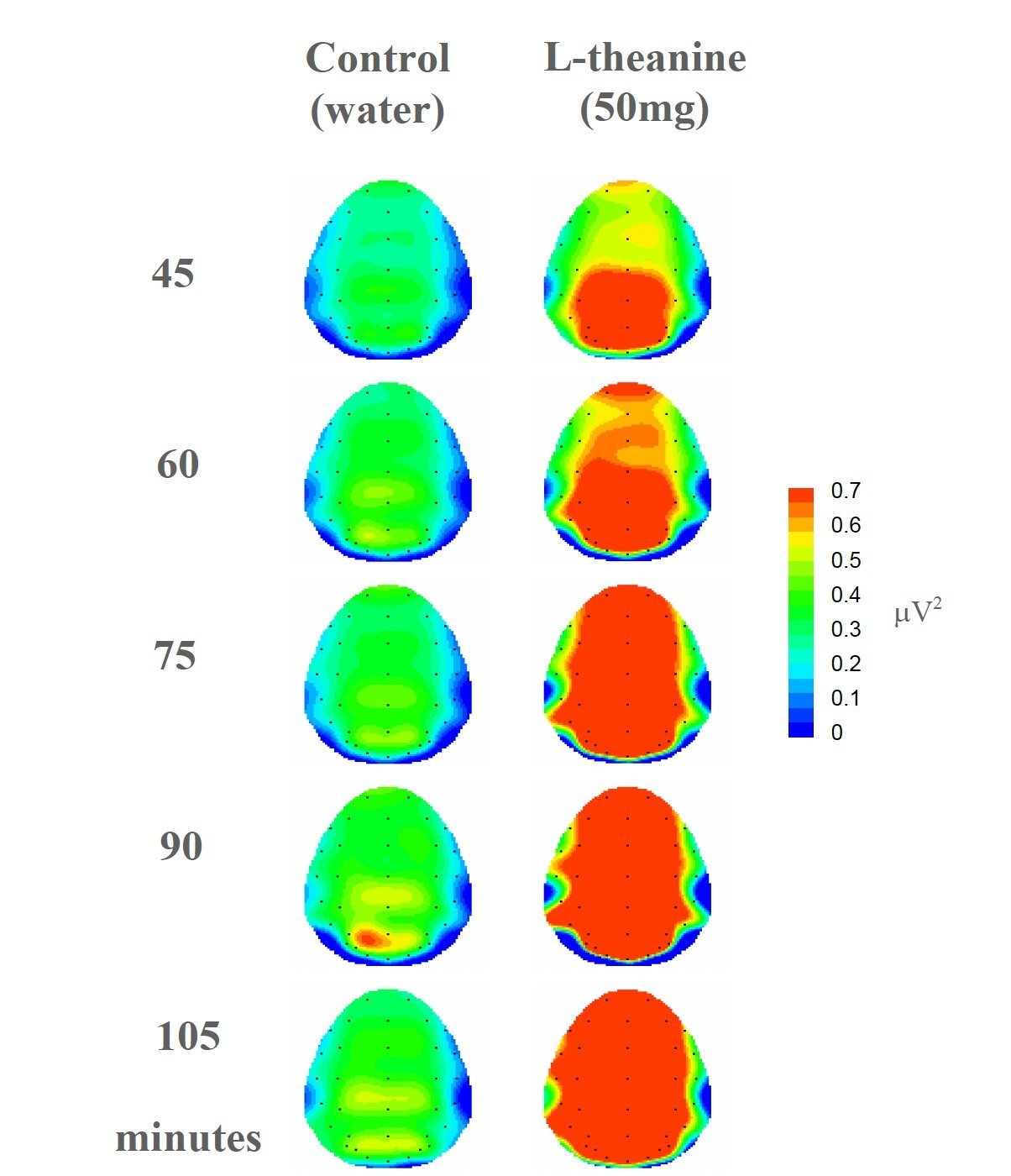
Rather than simply “calming” in a general sense, L-theanine seems to support a state of calm alertness, as reflected in the increased alpha-1 activity observed here. In a picture such as ADHD, where the problem is not always lack of activation but sometimes poorly coordinated activation, this nuance matters.
Red = more alpha-1 activity. Green = less alpha-1 activity. In this study, more red after taking L-theanine suggests a state of calm alertness, not sleepiness.
Figure adapted from:Nobre et al., Asia Pac J Clin Nutr.2008:17 Suppl 1:167-8, under a Creative Commons CC BY 4.0 licence.
Vitamin D
Vitamin D is one of those nutrients where the observational signal seems more consistent than the intervention signal. Several meta-analyses show that children and adolescents with ADHD tend to have lower serum concentrations of 25(OH)D, vitamin D3, than controls, which makes it a nutrient worth paying attention to. But that does not mean, on its own, that low vitamin D is causing ADHD in a simple and direct way.
Most of this literature is paediatric, and low levels may also reflect less time outdoors, season, adiposity, diet quality, sleep, or general health patterns that accompany ADHD, rather than clearly acting as a causal trigger. For that reason, I see it as an interesting association, but not a self-explanatory one.
The vitamin D story becomes more clinically relevant when we look at supplementation trials, although I also think the findings are sometimes overstated. The meta-analysis by Gan and colleagues, published in 2019, pooled four randomised clinical trials, including 256 children in total, and found small but statistically significant improvements in total ADHD symptoms, inattention, hyperactivity and behaviour. ²⁰
For me, however, the key methodological detail is that the studies included in this review were adjunctive trials. In other words, vitamin D was added to methylphenidate. It was not used as a standalone treatment. The authors themselves were also cautious: the evidence remained limited, and no clear improvements were seen in more challenging or oppositional behaviour problems. I would therefore read this as a modest signal of possible usefulness as an adjunct in children, not as proof that vitamin D independently “treats ADHD”.
The trial by Elshorbagy and colleagues is also striking because it reported improvements in cognitive function and in several symptom domains in children with ADHD after vitamin D supplementation. ²¹ But again, this is a paediatric study, and as with the rest of this literature, it does not resolve the question in adults. That is the point I would continue to emphasise. We still do not have robust supplementation data in adults, so it does not feel scientifically careful to extrapolate directly from child trials to adults with different physiology, more coexisting conditions such as anxiety, depression and disordered eating patterns, different medication use and different life pressures.
My current feeling is that vitamin D makes more sense as an intervention guided by nutritional status and the possibility of deficiency, especially when low levels are plausible, than as a general supplement for anyone with ADHD. The 2024 umbrella review by Kitaneh and colleagues also points in that direction: there is a plausible relationship between vitamin D and ADHD, but there is still heterogeneity and a need for better studies, especially outside paediatric populations. ²²
Vitamin D: My verdict
For me, vitamin D makes more sense as a marker of physiological terrain worth checking when there are reasons to suspect low levels, rather than as a general supplement for anyone with ADHD.
Magnesium
Magnesium is a slightly different case. Here, the literature on nutritional “status” is probably more consistent than the intervention literature. Two meta-analyses found that children with ADHD tend to show lower serum magnesium levels, ²³ and one of them also observed lower levels in hair. ²⁴
Although this provides a plausible biochemical signal, the literature on magnesium is more methodologically messy than it may seem. The studies do not all measure the same thing: serum, plasma, hair, saliva, red blood cells or urine, and these matrices do not tell exactly the same story. A critical review by Robberecht and colleagues explains this point well, noting that intracellular magnesium may be a more useful indicator than serum magnesium alone, and that stimulant medication itself may influence circulating levels. ²⁵ In other words, even before talking about supplementation, the biomarker question is already less clean than some headlines suggest.
What keeps me cautious is that the supplementation literature is harder to interpret than the literature on levels. For example, the Robberecht review also notes that many magnesium trials are not “pure” magnesium trials, because the mineral was administered alongside omega-3s, zinc or other nutrients. This makes it very difficult to attribute an effect to a single component. Other studies reached similar conclusions several years ago: magnesium may help some children with ADHD, especially when there is deficiency or a high risk of deficiency, but the evidence is not strong enough to justify a routine recommendation. ²⁶
In other words, magnesium seems plausible, potentially relevant and worth assessing, but I would not yet present it as a widely evidence-backed treatment for ADHD itself.
Another important point here is the gap in adults. Most of the magnesium literature remains paediatric, and newer data in community samples are still preliminary. The 2025 article by Hunter and colleagues is useful because it tries to widen the lens beyond childhood, but it was a small, mixed sample of neurodivergent people, with only 10 adults, and not a specific ADHD intervention trial. ²⁷ This makes it valuable for generating hypotheses, but not for supporting firm treatment claims.
Magnesium: My verdict
For me, magnesium deserves attention mainly in context, especially where there is restrictive eating, sensory selectivity, poor sleep, chronic stress or lower intake, rather than as a specific treatment for ADHD itself.
Would you like to know more about magnesium-rich foods? Read this article from Healthline: 10 Magnesium-Rich Foods That Are Super Healthy.
The gut microbiome, probiotics and fermented foods
The literature on the gut and brain is fascinating, but this is one of the easiest areas to exaggerate. And believe me, because this is the field I have been working in for many years, and I increasingly hear and read a lot of nonsense with very little scientific basis.
The 2024 systematic review by Allahyari and colleagues concluded that probiotics and prebiotics may be beneficial as adjunctive therapies in ADHD, but also called for longer studies, with more participants, a wider age range and more varied assessment methods. ²⁸ That feels like a fair summary of where we are. There is promise, but there is still a lot we do not know.
Data in adults remain especially scarce. A good example is a 2025 systematic review on gut microbiota modulation in adults with ADHD, which ended up including only three randomised clinical trials. ²⁹ Among those studies, the double-blind adult trial by Schwartz and colleagues, published in 2024, is especially interesting because it reported less hyperactivity, fewer gastrointestinal symptoms and better academic performance after probiotic intervention, with younger age being one of the predictors of a more favourable response. ³⁰
That said, when we talk about the microbiota, not everything has to be reduced to a probiotic capsule. In my own research, I have also explored microbiota-targeted interventions through diet and fermented foods such as kefir. I am especially interested in this approach because it moves away from the idea of a miracle strain and closer to a lived, edible and potentially more integrated intestinal ecology.
First, we published a feasibility study in Pilot and Feasibility Studies, where we tested a microbiome-targeted dietary intervention in children with ADHD and observed that the approach was safe, tolerable and feasible, with good adherence and enough signal to justify a larger trial. ³¹ We then published the protocol for the randomised trial on kefir, behaviour, sleep and the microbiome in BMJ Open, precisely to study this kind of food-based intervention more rigorously. ³² More recently, the clinical trial results were published in BMC Psychiatry. ³³
I do not think these studies close the case, not at all, but they do help widen the conversation. Perhaps the future of this field does not lie only in isolated supplements, but also in broader, more food-based ways of modulating the gut-brain axis.
Probiotics: My verdict
For me, this is a very promising and biologically fascinating field, but still too heterogeneous and preliminary for us to talk about universal solutions. The most interesting thing may not be one specific strain, but a more ecological and food-based way of modulating the gut-brain axis.
In the end, a tool, not a solution
All of this is one of the reasons I keep returning to the bigger picture. A capsule can support one layer of the system, but however tempting it may be, or however much it is sold to you as part of a “premium protocol”, it can never be the whole system.
Let me give you a brief example to illustrate what I mean. Movement matters, not simply because exercise is “healthy”, but because it changes physiology in ways that are relevant for regulation. Recent reviews suggest that exercise may increase microbial diversity in adults, enhance short-chain fatty acid production, and support adaptation and mitochondrial biogenesis. ³⁴ ³⁵ In other words, movement is not only about muscles. It is about energy, gut-brain signalling and state change. That is a very different conversation, and a much truer one, than “go for a run and your ADHD will be fixed”.
So, with all this caution, where does it leave us? From where I write, I may sound cautious, yes, but I can assure you that I also feel hopeful. I think saffron is worth watching closely. I think pine bark extract is very interesting, especially in younger ADHDers. I think melatonin can be very relevant when nervous system dysregulation affects sleep timing. I also think vitamin D and magnesium make more sense when low levels are plausible, and that L-theanine may help some people, especially in relation to overstimulation. And, of course, having specialised in the microbiota and mental health, I find this field fascinating, although I must recognise that it is still young.
Above all, I think supplements can support a broader plan, but they cannot be the plan. And I say that as a researcher, as a clinician and as a neurodivergent person who has spent many years trying almost everything.
So, to finish, I do not think the question is “which supplement fixes ADHD?” but “what needs support in my body and mind, and what can this tool realistically contribute?” It is a less flashy question, but a much more useful one, because it leaves enough space for medication, therapy, food, movement, creativity and self-compassion to form part of the same conversation, which is where I think they belong.
With care,
If you are trying to decide more clearly what role supplements, food, medication or other forms of support may have in your specific case, my ADHD & Neurodivergence Wellbeing page explains how I work one-to-one.
Important note: This review comes from my professional and research interest in the field, as well as my educational and clinical experience. If you are considering any of these supplements in the context of a medical condition or pharmacological treatment, please discuss this first with your doctor or a qualified dietitian or nutrition professional.
References: The science informing this article
National Institute for Health and Care Excellence. (2018, actualizado 2019). Attention deficit hyperactivity disorder: Diagnosis and management (NICE Guideline NG87).https://www.nice.org.uk/guidance/ng87
Notas: Notes: This NICE clinical guideline from the UK sets out evidence-based recommendations for ADHD diagnosis and treatment across the lifespan. It highlights that pharmacological treatment, including methylphenidate and lisdexamfetamine in adults, should be integrated within a broader and personalised therapeutic plan.
Gillies, D., Leach, M. J., & Perez Algorta, G. (2023). Polyunsaturated fatty acids (PUFA) for attention deficit hyperactivity disorder (ADHD) in children and adolescents. The Cochrane database of systematic reviews, 4(4), CD007986. https://doi.org/10.1002/14651858.CD007986.pub3
Notes: This study matters because it acts as a necessary counterweight to the enthusiasm that often surrounds omega-3s in ADHD. As a Cochrane review, it offers a particularly rigorous and cautious reading of the evidence available in children and adolescents, and reminds us that “widely researched” is not the same as “clearly effective”. In the context of this article, it helps place omega-3s in a more honest position: as a potential support within a broader approach, not as a powerful solution or something easily extrapolated to adults.
Liu, T.-H., Wu, J.-Y., Huang, P.-Y., Lai, C.-C., Chang, J. P.-C., Lin, C.-H., & Su, K.-P. (2023). Omega-3 polyunsaturated fatty acids for core symptoms of attention-deficit/hyperactivity disorder: A meta-analysis of randomized controlled trials. Journal of Clinical Psychiatry, 84(5), 22r14772. https://doi.org/10.4088/JCP.22r14772
Notes: What is interesting about this meta-analysis is that the possible advantage of omega-3s appeared only in longer trials, lasting at least four months, and referred to core ADHD symptoms overall as a modest signal within the ADHD clinical picture itself. At the same time, the study does not allow us to say clearly which specific dimension, inattention, hyperactivity or impulsivity, benefited most from longer duration.
Chang, J. P., Su, K. P., Mondelli, V., & Pariante, C. M. (2018). Omega-3 Polyunsaturated Fatty Acids in Youths with Attention Deficit Hyperactivity Disorder: a Systematic Review and Meta-Analysis of Clinical Trials and Biological Studies. Neuropsychopharmacology : official publication of the American College of Neuropsychopharmacology, 43(3), 534–545. https://doi.org/10.1038/npp.2017.160
Notes: Chang et al. is important because it introduces a necessary nuance into a literature that, if viewed only through more recent reviews, might seem more negative than it really is. Its value lies in detecting a favourable signal in children and adolescents, both in clinical symptoms and in some attention measures, while also adding biological plausibility by showing lower DHA and EPA levels in young people with ADHD. This study supports a balanced position: omega-3s do not seem to be a powerful intervention, but they cannot be dismissed as irrelevant either, especially in younger populations and perhaps in longer trials.
Baziar, S., Aqamolaei, A., Khadem, E., Mortazavi, S. H., Naderi, S., Sahebolzamani, E., Mortezaei, A., Jalilevand, S., Mohammadi, M. R., Shahmirzadi, M., & Akhondzadeh, S. (2019). Crocus sativus L. Versus Methylphenidate in Treatment of Children with Attention-Deficit/Hyperactivity Disorder: A Randomized, Double-Blind Pilot Study. Journal of child and adolescent psychopharmacology, 29(3), 205–212. https://doi.org/10.1089/cap.2018.0146
Notes: This study is important because it was one of the first trials to directly compare saffron and methylphenidate in children with ADHD, using a randomised, double-blind design. Its main interest lies in suggesting possible comparable short-term efficacy, but because it was a pilot study, with a small sample and only in children and adolescents, its results should be read as a promising signal, not as definitive proof or something easily extrapolated to adults. That is why I insist that methodology and sample demographics are always key if we want to avoid exaggerating the results of a study, however promising it may look.
Blasco-Fontecilla, H., Moyano-Ramírez, E., Méndez-González, O., Rodrigo-Yanguas, M., Martin-Moratinos, M., & Bella-Fernández, M. (2022). Effectivity of Saffron Extract (Saffr'Activ) on Treatment for Children and Adolescents with Attention Deficit/Hyperactivity Disorder (ADHD): A Clinical Effectivity Study. Nutrients, 14(19), 4046. https://doi.org/10.3390/nu14194046
Notes: A suggestive study because it explores the potential of saffron in children and adolescents with ADHD and includes more objective measures than many similar studies. Even so, its non-randomised design means it must be interpreted cautiously: it offers an interesting signal, but not definitive proof, and not something easily extrapolated to adults.
Pazoki, B., Zandi, N., Assaf, Z., Sanjari Moghaddam, H., Zeinoddini, A., Mohammadi, M. R., & Akhondzadeh, S. (2022). Efficacy and safety of saffron as adjunctive therapy in adults with attention-deficit/hyperactivity disorder: A randomized, double-blind, placebo-controlled clinical trial. Advances in Integrative Medicine, 9(1), 37–43. https://doi.org/10.1016/j.aimed.2022.01.002
Notes: This study feels especially relevant to me because it moves the conversation on saffron from childhood into the adult population, which remains uncommon in this field. It also does not evaluate saffron as a substitute for medication, but as an add-on to methylphenidate, which makes the clinical question more realistic. Its main value is that it offers a promising signal in adults within a randomised, double-blind, placebo-controlled design. At the same time, it remains a small and short study, so I would read it as an interesting proof of concept, not as definitive confirmation of efficacy.
Seyedi-Sahebari, S., Farhang, S., Araj-Khodaei, M., Akhondzadeh, S., Naseri, A., Sanaie, S., & Frounchi, N. (2024). The Effects of Crocus sativus (Saffron) on ADHD: A Systematic Review. Journal of attention disorders, 28(1), 14–24. https://doi.org/10.1177/10870547231203176
Notes: A small review, yes, but useful precisely because of that. It reminds us that enthusiasm for saffron in ADHD still rests on a handful of studies, not a mountain of evidence. Promising, yes; mature, not yet. But with tolerability that, so far, seems reasonably good. And as an intervention based on a food traditionally used for centuries, if expectations are appropriate, it may be a relatively low-risk way to experiment.
Han, S., Cao, Y., Wu, X., Xu, J., Nie, Z., & Qiu, Y. (2024). New horizons for the study of saffron (Crocus sativus L.) and its active ingredients in the management of neurological and psychiatric disorders: A systematic review of clinical evidence and mechanisms. Phytotherapy research : PTR, 38(5), 2276–2302. https://doi.org/10.1002/ptr.8110
Notes: This review is interesting because it broadens the focus considerably and places ADHD within a wider clinical map. For precisely that reason, it needs to be read carefully: when the zoom is pulled back too far, the ADHD-specific detail can seem more solid than it really is.
Trebatická, J., Kopasová, S., Hradecná, Z., Cinovský, K., Skodácek, I., Suba, J., Muchová, J., Zitnanová, I., Waczulíková, I., Rohdewald, P., & Duracková, Z. (2006). Treatment of ADHD with French maritime pine bark extract, Pycnogenol. European child & adolescent psychiatry, 15(6), 329–335. https://doi.org/10.1007/s00787-006-0538-3.
Notes: This trial has almost historical value within this small niche, because it helped put pine bark extract on the ADHD map long before the topic became “fashionable”. It is also interesting that even then it pointed towards oxidative stress as part of the picture, something that today fits quite well with more systemic and less reductionist readings of ADHD, where inflammation and oxidative stress are considered potentially relevant layers.
Hsu, C. D., Hsieh, L. H., Chen, Y. L., Lin, I. C., Chen, Y. R., Chen, C. C., Shirakawa, H., & Yang, S. C. (2021). Complementary effects of pine bark extract supplementation on inattention, impulsivity, and antioxidative status in children with attention-deficit hyperactivity disorder: A double-blinded randomized placebo-controlled cross-over study. Phytotherapy research : PTR, 35(6), 3226–3235. https://doi.org/10.1002/ptr.7036
Notes: The most appealing aspect of this study is not only the crossover design, which allows each child to act partly as their own control, but also the attempt to connect behaviour and antioxidant status in the same work. I see it as a good example of an intuition running through this whole article: sometimes the most interesting changes do not happen at one single level, but in the conversation between symptoms, biology and context.
Weyns, A.-S., Verlaet, A. A. J., Breynaert, A., Naessens, T., Fransen, E., Verhelst, H., Van West, D., Van Ingelghem, I., Jonckheere, A. I., Beysen, D., Kenis, S., Moens, E., van Roest, A. P. J., Savelkoul, H. F. J., De Bruyne, T., Pieters, L., Ceulemans, B., & Hermans, N. (2022). Clinical investigation of French maritime pine bark extract on attention-deficit hyperactivity disorder as compared to methylphenidate and placebo: Part 1: Efficacy in a randomised trial. Journal of Functional Foods, 97, 105246. https://doi.org/10.1016/j.jff.2022.105246
Notes: This study is particularly useful because it introduces a more demanding comparison than usual: not only against placebo, but also against methylphenidate. That forces pine bark extract into a more clinical and less idealised space. It does not make it a substitute for anything, but it does move it out of the purely speculative drawer.Weyns, A.-S., Verlaet, A. A. J., Van Herreweghe, M., Breynaert, A., Fransen, E., De Meester, I., Logie, E., Vanden Berghe, W., Verhelst, H., Van West, D., Van Ingelghem, I., Jonckheere, A. I., Beysen, D., Kenis, S., Moens, E., van Roest, A. P. J., Savelkoul, H. F. J., De Bruyne, T., Pieters, L., Ceulemans, B., & Hermans, N. (2022). Clinical investigation of French maritime pine bark extract on attention-deficit hyperactivity disorder as compared to methylphenidate and placebo: Part 2: Oxidative stress and immunological modulation. Journal of Functional Foods, 97, 105247. https://doi.org/10.1016/j.jff.2022.105247
Notes: I like this second article by Weyns and colleagues because it complicates the story, and as a good ADHDer, I love a complicated story! In this case, making it more complicated is a virtue. Instead of confirming a neat and elegant mechanism, it shows how difficult it is to robustly demonstrate that a compound acts exactly where we suspect it might act. Biology is often more tangled and less elegant than the hypotheses scientists create, and precisely for that reason, it feels more believable.Tenenbaum, S., Paull, J. C., Sparrow, E. P., Dodd, D. K., & Green, L. (2002). An experimental comparison of Pycnogenol and methylphenidate in adults with Attention-Deficit/Hyperactivity Disorder (ADHD). Journal of attention disorders, 6(2), 49–60. https://doi.org/10.1177/108705470200600201.
Checa-Ros, A., Muñoz-Hoyos, A., Molina-Carballo, A., Viejo-Boyano, I., Chacín, M., Bermúdez, V., & D'Marco, L. (2023). Low Doses of Melatonin to Improve Sleep in Children with ADHD: An Open-Label Trial. Children (Basel, Switzerland), 10(7), 1121. https://doi.org/10.3390/children10071121
Notas: Este estudio me parece útil porque pone el foco en algo que a menudo queda en segundo plano en el TDAH, el sueño. También recuerda que mejorar el descanso puede ser clínicamente relevante aunque no estemos “tratando el TDAH” de forma directa. Al ser un estudio abierto, yo lo leería como una señal inicial interesante, más orientada a abrir preguntas buenas que a cerrar conclusiones.van Andel, E., Bijlenga, D., Vogel, S. W. N., Beekman, A. T. F., & Kooij, J. J. S. (2021). Effects of chronotherapy on circadian rhythm and ADHD symptoms in adults with attention-deficit/hyperactivity disorder and delayed sleep phase syndrome: a randomized clinical trial. Chronobiology international, 38(2), 260–269. https://doi.org/10.1080/07420528.2020.1835943
Notas: Este estudio me parece especialmente valioso porque desplaza la conversación desde el “déficit de atención” hacia algo mucho más basal y corporal, el ritmo circadiano. En adultos con TDAH y síndrome de fase de sueño retrasada, recuerda que a veces parte del sufrimiento no está solo en la atención en sí, sino en vivir fisiológicamente desacompasados. También me gusta porque no presenta la cronoterapia como una solución mágica, sino como una vía interesante para pensar el TDAH desde la temporalidad, el sueño y la regulación, algo de lo que hablo en mi libro Cuerpo y Mente TDAH.Larsson, I., Aili, K., Lönn, M., Svedberg, P., Nygren, J. M., Ivarsson, A., & Johansson, P. (2023). Sleep interventions for children with attention deficit hyperactivity disorder (ADHD): A systematic literature review. Sleep medicine, 102, 64–75. https://doi.org/10.1016/j.sleep.2022.12.021
Notas: Una revisión especialmente útil porque recuerda que intervenir sobre el sueño no es “tratar algo aparte”, sino trabajar sobre una capa muy relevante para los que vivimos con TDAH. Su principal fuerza está en poner orden en un campo prometedor, pero todavía desigual y un tanto enmarañado en cuanto a métodos y resultados.Lyon, M. R., Kapoor, M. P., & Juneja, L. R. (2011). The effects of L-theanine (Suntheanine®) on objective sleep quality in boys with attention deficit hyperactivity disorder (ADHD): a randomized, double-blind, placebo-controlled clinical trial. Alternative medicine review : a journal of clinical therapeutic, 16(4), 348–354.
Notas: Este estudio me parece interesante porque sitúa la L-teanina en un lugar más realista y, para mí, más útil: no tanto como “suplemento para el TDAH” en sentido amplio, sino como posible apoyo para una capa concreta del cuadro, el sueño. También recuerda algo importante en este artículo: a veces mejorar el descanso no resuelve el TDAH, pero sí puede suavizar bastante la experiencia de vivir con él. Yo llevo tiempo tomando 400mg cada tarde/noche.Moshfeghinia, R., Sanaei, E., Mostafavi, S., Assadian, K., Sanaei, A., & Ayano, G. (2024). The effects of L-theanine supplementation on the outcomes of patients with mental disorders: a systematic review. BMC psychiatry, 24(1), 886. https://doi.org/10.1186/s12888-024-06285-y
Notas: Esta revisión me parece útil porque coloca la L-teanina en un lugar más realista: no como solución estrella, sino como apoyo suave y potencialmente interesante en cuadros donde la ansiedad, la sobreestimulación o el mal sueño forman parte del problema. También viene bien para recordar que tenemos que ser bastante prudentes al extrapolar desde “trastornos mentales” en general al TDAH en adultos.Gan, J., Galer, P., Ma, D., Chen, C. y Xiong, T. (2019). The Effect of Vitamin D Supplementation on Attention-Deficit/Hyperactivity Disorder: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Journal of Child and Adolescent Psychopharmacology, 29(9), 670–687.
Notas: Un metaanálisis importante porque ayuda a aterrizar la conversación sobre vitamina D: hay una señal pequeña a favor, sí, pero en ensayos pediátricos y como complemento al metilfenidato, no como tratamiento independiente. Su principal valor está en obligarnos a distinguir entre una ayuda coadyuvante plausible y una intervención principal, que sería decir demasiado. Elshorbagy, H.H., Barseem, N.F., Abdelghani, W.E. et al. (2018). Impact of Vitamin D Supplementation on Attention-Deficit Hyperactivity Disorder in Children. Annals of Pharmacotherapy, 52(7), 623–631.
Notas: Este estudio resulta interesante porque apunta a mejoras cognitivas y conductuales tras suplementación con vitamina D en niños, pero también porque ilustra bien uno de los límites recurrentes de este campo: los resultados son sugerentes en población pediátrica, sin resolver por ello la gran pregunta de si algo parecido ocurre en adultos. Es un estudio que abre una puerta, no que cierre el debate.Kitaneh, R., Jalilian-Khave, L., Ysrayl, B.B. et al. (2024). The Relationship Between Vitamin D and the Development and Treatment of Attention-Deficit Hyperactivity Disorder: An Overview of Systematic Reviews. Current Behavioral Neuroscience Reports, 11(3), 164–181.
Notas: Esta revisión paraguas me parece especialmente útil porque no intenta simplificar una literatura que sigue siendo bastante heterogénea. Más que vender una conclusión rotunda, ayuda a situar la vitamina D donde probablemente corresponde ahora mismo: como un factor biológicamente plausible y clínicamente interesante, pero todavía lejos de justificar un entusiasmo excesivo.Effatpanah, M., Rezaei, M., Effatpanah, H. et al. (2019). Magnesium status and attention deficit hyperactivity disorder (ADHD): A meta-analysis. Psychiatry Research, 274, 228–234.
Notas: Un metaanálisis útil porque refuerza la idea de que el magnesio merece atención como marcador biológico, aunque no necesariamente como solución terapéutica en sí misma. También es una buena advertencia contra las lecturas rápidas: la señal existe, pero la heterogeneidad entre estudios sigue siendo demasiado alta como para sacar conclusiones facilonas.Huang, Y.H., Zeng, B.Y., Li, D.J. et al. (2019). Significantly lower serum and hair magnesium levels in children with attention deficit hyperactivity disorder than controls: A systematic review and meta-analysis. Progress in Neuro-Psychopharmacology and Biological Psychiatry, 90, 134–141.
Notas: Lo más valioso de esta revisión, para mí, es que amplía la conversación más allá del suero e incluye también niveles en cabello, recordándonos que el “estado de magnesio” no siempre se deja capturar por un solo biomarcador. Aporta una señal consistente en niños, sí, pero también deja claro que medir no es lo mismo que saber exactamente qué hacer clínicamente con esa información. El valor está en poder traducir estos datos en una intervención clínica, pero todavía nos falta claridad.Robberecht, H., Verlaet, A.A.J., Breynaert, A., De Bruyne, T. y Hermans, N. (2020). Magnesium, Iron, Zinc, Copper and Selenium Status in Attention-Deficit/Hyperactivity Disorder (ADHD). Molecules, 25(19), 4440.
Notas: Esta revisión me gusta porque introduce una capa de complejidad muy necesaria. En lugar de asumir que “bajo en sangre” equivale automáticamente a “déficit clínico” o a “necesita suplemento”, recuerda que los biomarcadores minerales cuentan historias parciales y a veces contradictorias. En un campo tan proclive a simplificarse en redes, ese matiz vale mucho. La ciencia no es siempre fácil de simplificar a historias de Instagram…Lange, K.W., Hauser, J., Lange, K.M. et al. (2017). The Role of Nutritional Supplements in the Treatment of ADHD: What the Evidence Says. Current Psychiatry Reports, 19(2), 8.
Notas: Un artículo de revisión especialmente útil como mapa general, porque pone bastante orden en un terreno donde es fácil mezclar plausibilidad biológica con eficacia clínica probada. Su tono prudente sigue siendo muy vigente: algunos nutrientes pueden ayudar en contextos concretos, pero la evidencia dista mucho de sostener promesas amplias o soluciones fáciles.Hunter, C., Smith, C., Davies, E., Dyall, S.C. y Gow, R.V. (2025). A closer look at the role of nutrition in children and adults with ADHD and neurodivergence. Frontiers in Nutrition, 12, 1586925.
Notas: Este trabajo me parece interesante porque intenta abrir la conversación nutricional más allá del TDAH infantil puro y duro, incorporando también adultos y otras formas de neurodivergencia. Justamente por eso conviene leerlo como lo que es: una pieza preliminar, útil para generar preguntas y detectar patrones, pero no para sostener afirmaciones clínicas fuertes por sí sola. Desde luego, no es un artículo que nos sirva para crear un “protocolo nutricional para el TDAH”.Allahyari, P., Abbas Torki, S., Aminnezhad Kavkani, B., Mahmoudi, Z., Mousavi Hoseini, M. S., Moradi, M., Alami, F., Keshavarz Mohammadian, M., Bahoo Sele Bani, S., Abbasi Mobarakeh, K., Shafaei, H., Khoshdooz, S., Hajipour, A., Doaei, S., & Gholamalizadeh, M. (2024). A systematic review of the beneficial effects of prebiotics, probiotics, and synbiotics on ADHD. Neuropsychopharmacology reports, 44(2), 300–307. https://doi.org/10.1002/npr2.12437
Notas: Una revisión útil porque resume bien el momento actual del campo: hay señales prometedoras, pero todavía demasiado enmarañamiento en cepas, duración, edad y medidas de resultado como para hablar con excesiva seguridad. En otras palabras, interesante, sí; listo para simplificaciones comerciales, no.Gomes, A., Soares, A., Correia, C. G., Castelo-Branco, M., & Oliveira, G. (2025). The effectiveness of the gut microbiota modulation on ADHD in adults: A systematic review. Current Developmental Disorders Reports. Advance online publication. https://doi.org/10.1007/s40501-025-00358-9
Notas: Esta revisión me parece muy valiosa precisamente porque baja el volumen del entusiasmo. En adultos con TDAH, el campo sigue siendo tan pequeño que una revisión sistemática acaba trabajando con apenas tres ensayos aleatorizados. A veces, el dato más importante de una revisión no es lo que confirma, sino lo poco que todavía sabemos.Levy Schwartz, M., Magzal, F., Yehuda, I., & Tamir, S. (2024). Exploring the impact of probiotics on adult ADHD management through a double-blind RCT. Scientific reports, 14(1), 26830. https://doi.org/10.1038/s41598-024-73874-y
Notas: Me parece uno de los estudios más interesantes en adultos, no porque resuelva el tema, sino porque conecta síntomas de TDAH, síntomas gastrointestinales y rendimiento funcional dentro del mismo ensayo. También me gusta que encuentre una respuesta más favorable en participantes más jóvenes, porque sugiere que la historia quizá no vaya solo de “si funciona o no”, sino también de cuándo, en quién y bajo qué condiciones. Los matices son lo que más me fascina de la ciencia según se va desplegando en campos tan complejos como este.Lawrence, K., Myrissa, K., Toribio-Mateas, M., Minini, L., & Gregory, A. M. (2022). Trialling a microbiome-targeted dietary intervention in children with ADHD-the rationale and a non-randomised feasibility study. Pilot and feasibility studies, 8(1), 108. https://doi.org/10.1186/s40814-022-01058-4
Notas: Para mí, este estudio tiene valor porque cambia el foco desde el suplemento aislado hacia una intervención alimentaria dirigida a la microbiota. No intenta demostrar demasiado pronto una eficacia espectacular; hace algo más importante al principio de un programa de investigación: comprobar si el enfoque es viable, seguro y razonablemente habitable en la vida real. Además soy uno de los autores, y fue una experiencia enriquecedora trabajar en el diseño, la realización del estudio y la interpretación de los datos.Lawrence, K., Fibert, P., Hobbs, J., Myrissa, K., Toribio-Mateas, M. A., Quadt, F., Cotter, P. D., & Gregory, A. M. (2023). Randomised controlled trial of the effects of kefir on behaviour, sleep and the microbiome in children with ADHD: a study protocol. BMJ open, 13(12), e071063. https://doi.org/10.1136/bmjopen-2022-071063
Notas: Aunque sea un protocolo, me parece una referencia importante porque muestra ambición metodológica y claridad conceptual. Sitúa el kéfir no como un “probiótico natural” sin más, sino como una intervención alimentaria compleja, con potencial para influir en conducta, sueño y microbioma dentro de un diseño más riguroso. Igualmente soy uno de los autores y la razón por la que se publicó es muy importante. Aprendimos mucho en nuestro estudio preliminar, con lo cual necesitábamos ser transparentes con la comunidad científica y admitir que algunas de nuestras suposiciones no eran correctas, y que los métodos que habíamos utilizado en el estudio de factibilidad no eran los más adecuados.Lawrence, K., Fibert, P., Toribio-Mateas, M., Gregory, A. M., Hobbs, J., Quadt, F., Wright, S., Cotter, P. D., Patel, S., & Myrissa, K. (2025). Effects of kefir on symptoms, sleep, and gut microbiota in children with ADHD: a randomised controlled trial. BMC psychiatry, 25(1), 1117. https://doi.org/10.1186/s12888-025-07568-8
Notas: Este ensayo me parece especialmente valioso porque nos permitió llevar la conversación un paso más allá del “probiotic pill mindset” y estudiar un alimento fermentado completo en un ensayo controlado. Lo que más me interesa no es vender el kéfir como solución, sino abrir una vía más ecológica y más alimentaria para pensar la modulación del eje intestino-cerebro en TDAH. Estoy muy orgulloso del trabajo que mis compañeros y yo hicimos, y de haber podido publicarlo en una revista de psiquiatría tan eminente.Min, L., Ablitip, A., Wang, R., Luciana, T., Wei, M., & Ma, X. (2024). Effects of Exercise on Gut Microbiota of Adults: A Systematic Review and Meta-Analysis. Nutrients, 16(7), 1070. https://doi.org/10.3390/nu16071070
Notas: Esta revisión me parece útil porque refuerza una de las ideas centrales de este artículo: el movimiento no beneficia solo al músculo o al ánimo, también parece dialogar con la ecología intestinal. Tengo que ser honesto y decir que no convierte el ejercicio en una panacea, pero sí ayuda a pensar en el cuerpo como una red de sistemas con el potencial de influirse y beneficiarse entre ellos.Al-Beltagi, M., Saeed, N. K., Bediwy, A. S., El-Sawaf, Y., Elbatarny, A., & Elbeltagi, R. (2025). Exploring the gut-exercise link: A systematic review of gastrointestinal disorders in physical activity. World journal of gastroenterology, 31(22), 106835. https://doi.org/10.3748/wjg.v31.i22.106835
Notas: Me parece una revisión interesante porque amplía la conversación entre ejercicio e intestino más allá de la microbiota aislada y la sitúa dentro de una fisiología más global. En el contexto de este artículo, ayuda a sostener la idea de que moverse afecta mucho más que el gasto energético, modificando el terreno corporal desde el que vivimos el TDAH.